Can Rubella Cause Autism?
The topic of whether rubella can cause autism is essential for parents to understand, as it may impact their decision-making regarding vaccines and prenatal care.
Can Rubella Cause Autism?
In this blog post, we will explore the relationship between rubella and autism. The topic of whether rubella can cause autism is essential for parents to understand, as it may impact their decision-making regarding vaccines and prenatal care. We will delve into the scientific evidence and studies conducted on this subject, providing a comprehensive analysis to help you make informed decisions.
What is Rubella?
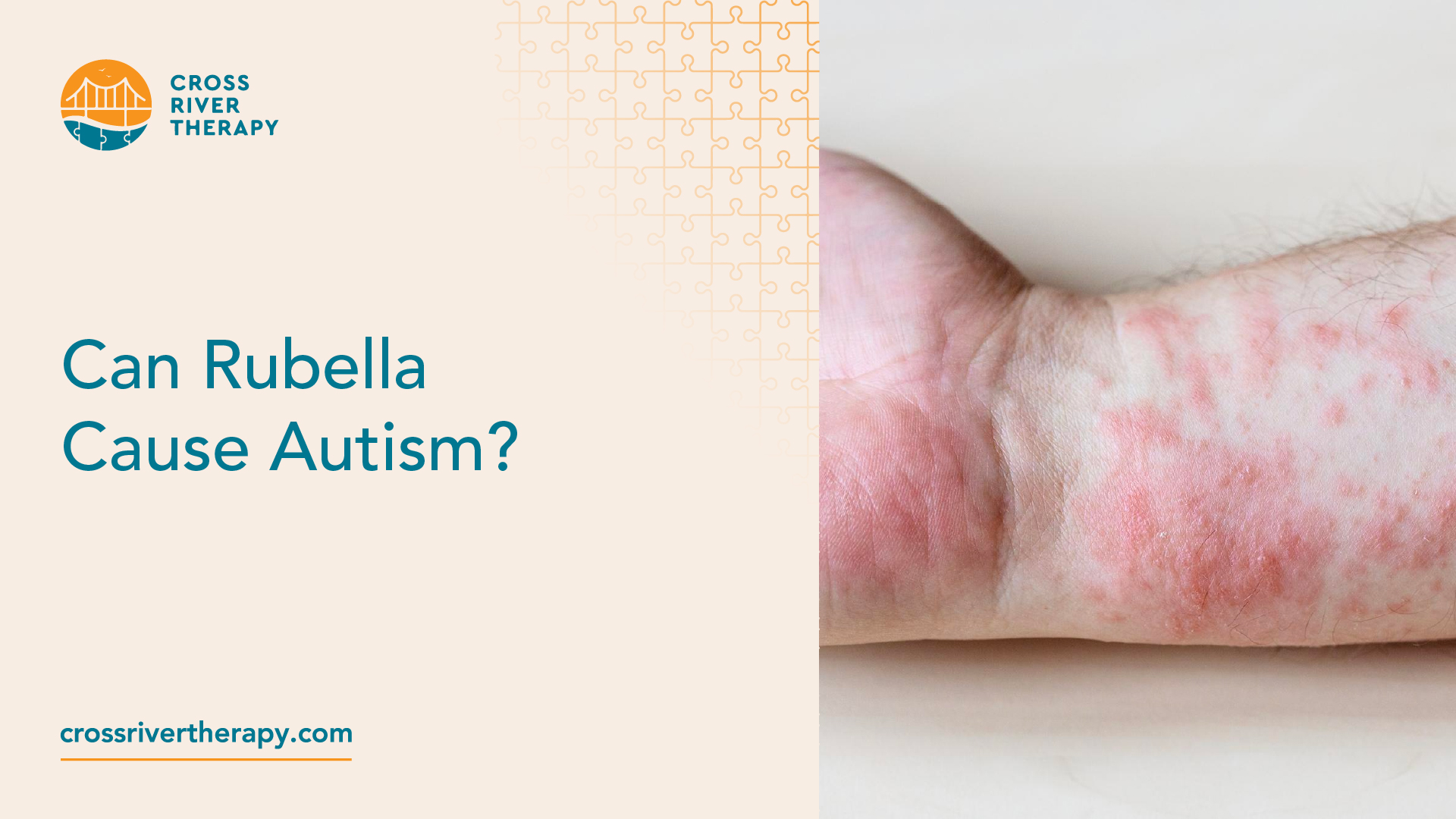
Rubella, also known as German measles, is a viral infection that primarily affects the skin and lymph nodes. It is characterized by a distinctive red rash and mild symptoms such as fever, headache, and swollen lymph nodes.
While rubella is generally a mild illness in children, it can have severe consequences for pregnant women, leading to miscarriages, stillbirths, or severe birth defects known as Congenital Rubella Syndrome (CRS).
Congenital Rubella Syndrome (CRS)
CRS occurs when a pregnant woman contracts rubella during the first 20 weeks of pregnancy. The virus can cross the placenta and infect the developing fetus, causing a range of birth defects, including:
- Deafness
- Cataracts
- Heart defects
- Intellectual disabilities
- Liver and spleen damage
The History of Rubella and Its Impact on Public Health Before Vaccination
Before the development of the rubella vaccine, rubella outbreaks were common and had significant consequences for public health. In the early 20th century, rubella was considered a relatively harmless childhood illness.
However, this perception changed in the 1940s when Australian ophthalmologist Sir Norman Gregg discovered a link between maternal rubella infection and congenital cataracts in infants.
Further research revealed that rubella infection during pregnancy could lead to a wide range of birth defects, collectively referred to as Congenital Rubella Syndrome (CRS). This discovery led to increased awareness about the dangers of rubella, especially for pregnant women.
One of the most significant rubella epidemics occurred in the United States between 1964 and 1965. During this period, approximately 12.5 million cases of rubella were reported, resulting in an estimated 20,000 CRS-affected infants born with severe disabilities. This outbreak highlighted the urgent need for a preventative measure against rubella.
In response to this crisis, scientists developed a live attenuated rubella vaccine that was introduced in 1969. The widespread use of this vaccine led to a dramatic decline in both rubella infections and CRS cases.
Today, thanks to effective vaccination programs, rubella is considered eliminated from many countries, including the United States. However, it remains crucial to maintain high vaccination rates to prevent future outbreaks and protect vulnerable populations from this once-devastating disease.
The Rubella Vaccine and Autism
The rubella vaccine is included in the MMR (measles, mumps, and rubella) vaccine, which is administered to children in most countries as part of routine immunization programs. This vaccine has been the subject of controversy due to a now-debunked study published in 1998, which claimed a link between the MMR vaccine and autism.
Numerous studies since then have consistently shown no connection between the MMR vaccine and autism. In 2019, a comprehensive study involving over 650,000 children confirmed that there is no increased risk of autism among children who receive the MMR vaccine.
Can Rubella Itself Cause Autism?
While the MMR vaccine has been proven not to cause autism, the question remains whether rubella infection itself can lead to autism spectrum disorder (ASD). Some studies have suggested a possible link between maternal rubella infection and an increased risk of autism in the offspring.
A review of studies published in 2015 found that children born to mothers who had rubella during pregnancy were at a higher risk of developing autism.
However, these findings do not establish a direct cause-and-effect relationship between rubella and autism. It is possible that other factors, such as genetic predisposition or environmental influences, contribute to the increased risk of ASD in these cases.
Addressing Common Misconceptions About Vaccines and the MMR Vaccine
Misconception 1: Vaccines Cause Autism
As mentioned earlier, there is no scientific evidence linking vaccines to autism. The original study that claimed a connection between the MMR vaccine and autism has been thoroughly discredited and retracted. Numerous large-scale studies have consistently found no association between vaccines and autism.
Misconception 2: Too Many Vaccines Overwhelm the Immune System
The human immune system is capable of handling numerous antigens (substances that trigger an immune response) at once. In fact, babies are exposed to countless antigens in their daily lives from the moment they are born.
The number of antigens in vaccines is minuscule compared to what children encounter naturally. Modern vaccines are designed to be efficient and safe, stimulating a protective immune response without overwhelming the immune system.
Misconception 3: Natural Immunity Is Better Than Vaccine-Induced Immunity
While natural immunity can sometimes provide stronger or longer-lasting protection than vaccines, it often comes with significant risks.
For example, contracting rubella during pregnancy can lead to severe birth defects or even death for the unborn child. On the other hand, vaccination offers a safer way to develop immunity without exposing individuals to potentially life-threatening diseases.
Misconception 4: Vaccines Contain Harmful Ingredients
Vaccine ingredients are carefully chosen for their safety and effectiveness in promoting an immune response.
Some people may raise concerns about ingredients such as thimerosal (a mercury-based preservative) or aluminum salts (used as adjuvants). However, these substances have been extensively studied for their safety at the levels used in vaccines.
Thimerosal has been removed or reduced to trace amounts in most childhood vaccines due to public concern, although no scientific evidence supports a link between thimerosal-containing vaccines and developmental disorders like autism. Aluminum salts used as adjuvants in vaccines have a long history of safe use and are present in amounts far below the daily intake from food and water.
By addressing these common misconceptions, we can help build confidence in the safety and efficacy of vaccines, including the MMR vaccine, which plays a crucial role in protecting public health.
Global Efforts to Eliminate Rubella Through Vaccination Programs
In response to the devastating effects of rubella and CRS, global health organizations have joined forces to eliminate rubella through widespread vaccination programs. These initiatives aim to reduce the incidence of rubella and CRS worldwide and protect vulnerable populations from this preventable disease.
World Health Organization (WHO) Strategy for Rubella Elimination
The World Health Organization (WHO) has developed a comprehensive strategy for eliminating rubella and preventing CRS. This strategy includes:
- High vaccination coverage: Ensuring that at least 95% of children receive two doses of the MMR vaccine.
- Surveillance: Monitoring rubella cases and identifying outbreaks promptly.
- Response: Implementing rapid responses to control outbreaks when they occur.
By following these guidelines, several countries have successfully eliminated rubella, demonstrating that a global elimination is achievable with concerted efforts.
GAVI, the Vaccine Alliance
GAVI, the Vaccine Alliance, is an international organization committed to improving access to vaccines in low-income countries. Since its inception in 2000, GAVI has supported the introduction of the MMR vaccine in over 50 countries, resulting in a significant reduction in rubella cases worldwide.
Through funding and partnerships with governments and other organizations, GAVI continues to play a crucial role in expanding access to vaccines and achieving global rubella elimination.
Regional Initiatives for Rubella Elimination
In addition to global efforts led by WHO and GAVI, regional initiatives also contribute significantly towards eradicating rubella. For example:
- The Pan American Health Organization (PAHO) launched an initiative in 1997 targeting measles elimination in Latin America. In 2003, PAHO expanded this program to include rubella elimination. As a result of these efforts, both measles and rubella were declared eliminated from the Americas in 2016.
- The European Regional Office of WHO has set a goal to eliminate rubella in the European Region by 2020. Although this target has not yet been achieved, significant progress has been made in recent years.
Through these global and regional efforts, rubella elimination is becoming an increasingly attainable goal. Continued dedication to vaccination programs and surveillance will be essential for maintaining progress and ensuring that future generations are protected from the devastating effects of rubella and CRS.
Why Vaccination is Important?
- Prevents life-threatening diseases: Vaccines protect individuals from a variety of severe and potentially fatal diseases, reducing the risk of illness and death.
- Herd immunity: When a significant portion of a population is vaccinated, it becomes difficult for infectious diseases to spread within that community. This protects those who cannot be vaccinated, such as infants, pregnant women, or individuals with compromised immune systems.
- Eradication of diseases: High vaccination coverage can lead to the eradication of certain diseases, such as smallpox. This eliminates the need for future vaccinations against that disease.
- Reduced healthcare costs: Vaccination helps prevent costly medical treatments and hospitalizations associated with vaccine-preventable diseases, saving both individuals and governments money.
- Prevention of complications: Some vaccine-preventable diseases can cause long-term health complications. Vaccination helps prevent these complications, improving overall quality of life.
- Safe and effective: Vaccines go through rigorous testing before they are approved for use, making them a safe and effective way to protect against infectious diseases.
Analyzing the Impact of Rubella Vaccination Programs on Autism Diagnosis
As rubella vaccination programs have become more widespread, some have raised concerns about a potential link between the vaccine and autism. However, numerous studies have consistently shown no connection between the MMR vaccine (which includes rubella) and autism.
In fact, some researchers have suggested that widespread vaccination programs may actually contribute to lower rates of autism diagnosis. A study published in 2019 found that areas with higher MMR vaccination rates had lower rates of autism diagnosis, suggesting that vaccines may play a protective role against autism.
While the exact mechanisms underlying this association are not yet fully understood, it is clear that rubella vaccination programs do not increase the risk of autism and may even help prevent it. By providing protection against rubella and other infectious diseases, vaccines can help ensure healthier outcomes for all individuals.
FAQs
Is there a link between rubella and autism?
Some studies have suggested a possible association between maternal rubella infection during pregnancy and an increased risk of autism in the offspring.
However, these findings do not establish a direct cause-and-effect relationship between rubella and autism. More research is needed to better understand the potential links between rubella and autism.
Can rubella vaccination cause autism?
No, the rubella vaccine (or any vaccine) has been proven not to cause autism. Numerous large-scale studies have consistently found no association between vaccines and autism.
If I am planning to get pregnant, should I be concerned about rubella?
Yes, if you are planning to become pregnant, it is essential to make sure you are immune to rubella before conceiving. If you contract rubella during pregnancy, it can lead to severe birth defects or even death for the unborn child. You can check your immunity status by getting a blood test from your healthcare provider.
How does the MMR vaccine protect against rubella?
The MMR vaccine contains weakened live viruses that stimulate the body's immune system to produce protective antibodies against measles, mumps, and rubella. After receiving the vaccine, if an individual comes into contact with these viruses again in the future, their immune system will recognize them and produce antibodies quickly, preventing illness.
Why is it important for everyone to get vaccinated against rubella?
Vaccination is crucial for protecting both individuals and communities from infectious diseases like rubella. When a significant portion of a population is vaccinated (a concept known as herd immunity), it becomes difficult for infectious diseases like rubella to spread within that community.
This protects those who cannot be vaccinated due to medical reasons such as infants or individuals with compromised immune systems. Vaccination also helps prevent costly medical treatments and hospitalizations associated with vaccine-preventable diseases, saving both individuals and governments money.
Summary
While there is some evidence suggesting a possible link between maternal rubella infection and an increased risk of autism in offspring, further research is needed to establish a direct cause-and-effect relationship.
The MMR vaccine, which includes protection against rubella, has been proven not to cause autism and plays a vital role in preventing the severe consequences of rubella infection during pregnancy.



