51 PTSD Statistics & Facts: How Common Is PTSD?
Did you know that approximately 5% of Americans – more than 13 million people – have PTSD at any given time?

Key PTSD Statistics & Facts
- An estimated 70% of adults in the United States have experienced at least one traumatic event in their lifetime.
- Up to 20% of these people go on to develop post-traumatic stress disorder.
- An estimated 5% of Americans – more than 13 million people – have PTSD at any given time.
- Around 8.7% of all adults – 1 in 13 people in the U.S. will develop PTSD at some point in their lifetime.
- Around 3.6% of adults in the U.S. suffer from PTSD in a given year.
- Approximately 1 in 9 women will get PTSD at some point in their lifetime, and women are around twice as likely as men to develop the disorder.
- Surprisingly, 23% of women in the military report being sexually assaulted. And 55% of female veterans and 38% of male veterans experienced sexual harassment while in the military.
- Researchers found the estimated prevalence of PTSD among veterans ranges from 1.09% to 34.84%.
- Post-traumatic stress disorder (PTSD) can occur after any traumatic event, not only trauma from wartime.
- 16% of emergency physicians meet diagnostic criteria of PTSD.
- Around 5% of adolescents experience PTSD.

PTSD Prevalence: How Common Is PTSD?
Prevalence Of PTSD By Country

U.S PTSD Statistics

- Around 70% of adults in the United States have experienced at least one traumatic event in their lifetime.
- Up to 20% of these people go on to develop post-traumatic stress disorder.
- Approximately 5% of Americans – more than 13 million people – have PTSD at any given time.
- Approximately 8.7% of all adults – 1 in 13 people in the U.S. will develop PTSD at some point in their lifetime.
- Approximately 3.6% of adults in the U.S. suffer from PTSD in a given year.
- Of people in the U.S. who experience a traumatic event, 1 in 5 of them will develop the condition.
- 36.6% of PTSD cases are severe, 33.1% are moderate, and 30.2% are mild according to a study by Harvard Medical School in 2007.
Canada PTSD Statistics

- Canada has the highest rates of PTSD of 24 countries that were studied by the British Journal of Psychiatry in 2016.
- 9% of Canadians will suffer from PTSD in their lifetime.
PTSD Statistics By Gender

- Around 1 in 9 women will get PTSD at some point in their lifetime.
- Women are around twice as likely as men to develop the disorder.
- Surprisingly, 23% of women in the military report being sexually assaulted.
- 55% of female veterans and 38% of male veterans experienced sexual harassment while in the military.
PTSD Statistics By Age

- PTSD in adults was highest in 45- to 59-year-olds (5.3%) as of 2001-2003.
- PTSD in adolescents was highest in female adolescents aged 13 to 18 (8%) as of 2001-2004.
- PTSD prevalence was lowest in adults aged 60 or older (1%) as of 2001-2003.
PTSD Statistics By Race

- A study found that the lifetime prevalence of PTSD was highest among Blacks (8.7%), intermediate among Hispanics and Whites (7.0% and 7.4%) and lowest among Asians (4.0%).
PTSD Statistics By Trauma
Post-traumatic stress disorder is rooted in traumatic events, so we’ve compiled the latest data which illustrates the percentage of people who will likely develop the disorder after experiencing these traumatic events:
PTSD In Adults
In the past year, PTSD affected around 3.6% of American adults over the age of 18 according to studies.
The symptoms of PTSD in adults are grouped as serious, moderate or mild, and there are approximately 36.6% of adults who experience serious impairment, 33.1% of adults who experience a moderate impairment, and 30.2% of adults who experience mild impairment. All age groups can be affected even though most statistics focus on PTSD in adults.

It’s possible for the disorder to occur in children, though sometimes childhood trauma doesn’t result in the disorder until after the brain has more time to develop in the individual’s early adulthood.
PTSD Among Adolescents
Around 5% of adolescents experience PTSD. Studies on PTSD in teenagers have found that just 1.5% experience severe impairment. Unsurprisingly, PTSD in adolescents is more than twice as prevalent in the later teen years, as the prevalence of PTSD for teens aged 13-4 is 3.7%. In the 17-18 age group, the PTSD prevalence increases to 7%.

PTSD & Domestic Violence
The connection between PTSD and domestic violence is clear even if PTSD might not always develop immediately following abuse. There are several factors which influence the probability of domestic violence victims developing post traumatic stress disorder, including the severity and duration of violence, and the age of the victim.
Whether or not someone feels their life is in danger can also influence the chance of PTSD developing in the victim. The intense emotional connection victims might have with the abuser is probably a big part of what makes the violence such a traumatic experience for the victim.
Veteran PTSD Statistics
Many researchers have worked to understand the prevalence of PTSD among military veterans. The result of their efforts are statistics that we’ve compiled. Estimates of prevalence in veterans vary widely because the field of psychiatry has defined and assessed PTSD in multiple ways over time.
In one recent analysis of 32 scientific articles, researchers found the estimated prevalence of PTSD among veterans ranges from 1.09% to 34.84%.

A 2017 study involving 5,826 U.S. veterans showed that 12.9% were diagnosed with PTSD. This is a shockingly high prevalence rate compared to the prevalence of PTSD among the general population: only 8.7% of the U.S. population will experience PTSD in their lives. And around 3.6% of adults in the U.S. suffer from PTSD in a given year.
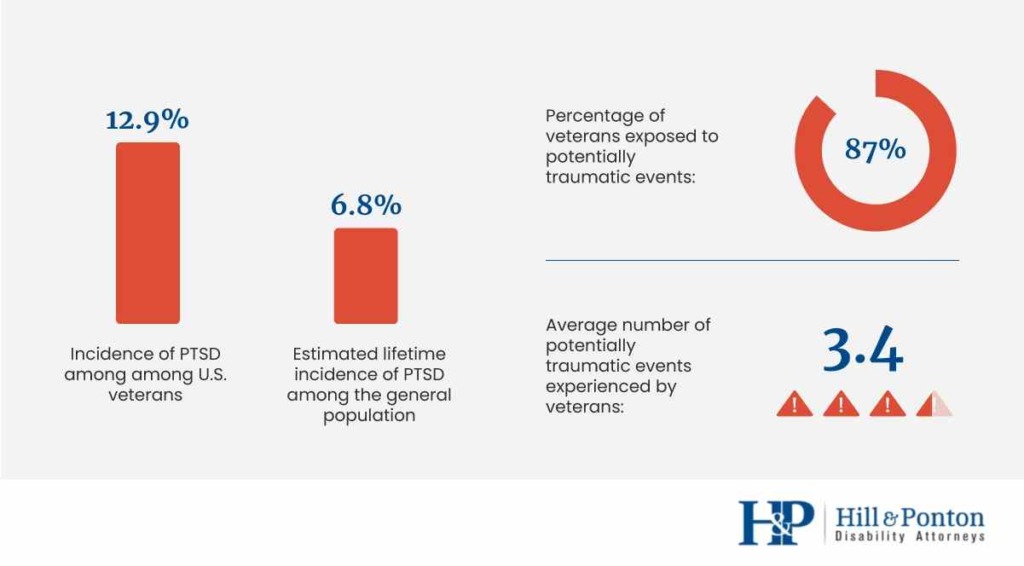
And in a 2014 study involving 3,157 U.S. veterans, 87% reported exposure to at least one potentially traumatic event in their lifetime. Veterans reported 3.4 potentially traumatic events during their lifetime, on average.
Surprisingly, nearly 1 in 4 women in the military report being sexually assaulted. And 55% of female veterans and 38% of male veterans experienced sexual harassment while in the military.

- Around 30% of Vietnam veterans have had PTSD in their lifetime. (according to American Psychological Association in 1990)
- Approximately 354 million adult war survivors globally have PTSD and/or major depression. (according to European Journal of Psychotraumatology in 2019)
- PTSD prevalence of around 14% was present in veterans who served in Iraq in one study of 1,938 veterans. (according to U.S. Department of Veterans Affairs)
- A 10% prevalence of PTSD has been extrapolated for all Gulf War veterans in a 2003 report by American Journal of Epidemiology.
PTSD Symptoms
PTSD symptoms may include unwanted memories of the trauma, avoidance of situations that bring back memories of the trauma, nightmares, anxiety, depressed mood, or heightened reactions.
People may experience these symptoms:
- Intrusion of thoughts, flashbacks, memories, and dreams
- Avoidance of reminders of traumatic events
- Alterations in mood and cognition
- Alterations in reactivity and arousal
- Insomnia or nightmares
- Emotional detachment or unwanted thoughts
- Self-destructive behavior, social isolation, irritability, agitation
- Loss of interest in activities, loneliness, or guilt

PTSD & Co-Occurring Conditions
It’s possible for many mental health disorders to co-occur with PTSD in part, to the significant changes in brain functioning following trauma that leads to the disorder. The most common conditions someone with PTSD may experience include:
- Depression
- Suicidal thoughts
- Trauma
- Anxiety
- Substance use disorders
We’ll go into more detail on each condition in this section.

PTSD & Depression
Approximately 1 in 10 people have some form of depressive disorder every year, making it a common mental health condition. It’s more common among people who’ve experienced traumatic experiences.
As mentioned earlier, PTSD and depression frequently co-occur. Specifically, people with PTSD are 3-5 times more likely to have depression.

PTSD & Suicide
In general, people diagnosed with PTSD who struggle to express their emotions have a higher risk of suicide. Other common co-occurring conditions such as depression or anxiety can make a negative impact on the chances of suicide for someone with the disorder.

PTSD & Trauma
Disruptions and changes in brain chemistry caused by an individuals’ trauma is the main reason why PTSD and trauma are interconnected. The condition can occur in response to traumas besides military combat (example: sexual abuse).
However, there are other traumatic events which can happen in a person’s life that might lead to the disorder:
- 49% of rape victims will develop PTSD.
- Almost 32% of physical assault victims will develop PTSD.
- 16.8% of people involved in serious vehicle accidents develop PTSD.
- 15.4% of shooting and stabbing victims develop PTSD.
- 14.3% of people who unexpectedly and suddenly experience the death of a close loved one develop PTSD.
- 7.3% of people who’ve witnessed the murder or serious injury of another person will develop PTSD.
- 3.8% of people who experience natural disasters develop PTSD.
PTSD & Anxiety
Currently, PTSD is considered a separate type of disorder, but in the past it was categorized as an anxiety disorder because PTSD and anxiety disorders share some symptoms, many of which can impair sleep and other biological functions. For example, someone with anxiety related to PTSD can frequently feel on edge and be easily startled.
Similarly, anxiety caused by the disorder can make it challenging for an individual to concentrate, and it can also increase their agitation.
PTSD & Substance Abuse
One study estimates that 46.4% of people diagnosed with the disorder also meet the criteria for a substance use disorder. Another study found that women with the disorder were 2.48 times more likely to suffer from alcohol abuse, while men with the disorder were 2.06 times more likely.

PTSD Treatment Statistics
Medication, psychotherapy, or a combination of both can treat PTSD. Even though there’s more than one type of psychotherapy used to treat the disorder, trauma-focused psychotherapies with a mental healthcare professional are the most recommended.
That’s primarily because this type of treatment assists people to process their experiences by helping them focus on the memory of the traumatic event or the meaning behind it.
In fact, studies have demonstrated that up to 46% of people diagnosed with the disorder show improvement within the first six weeks of psychotherapy.

Another treatment option that can alleviate the symptoms of PTSD, including anxiety, are antidepressants. Interestingly, studies show up to 62% of people who receive medication for PTSD show improvement. (American Family Physician, 2003)
First Responder PTSD Statistics
If you’re wondering how common is PTSD among first responders, this section will show you the up-to-date stats.
Surprisingly, more than 80% of first responders experience traumatic events on the job. The challenging and dangerous situations they face cause them to be at a high risk of developing PTSD as a work-related injury or condition.

In fact, according to the Substance Abuse and Mental Health Services Administration, an estimated 30% of first responders develop behavioral health conditions including, but not limited to, depression and PTSD, as compared with 20% in the general population.
9/11 PTSD Statistics

More than 21% of residents enrolled in the WTC Health Registry reported new PTSD symptoms 5 to 6 years after the tragic day. PTSD among residents increased from more than 13% 2-3 years after the attacks to more than 16% 5-6 years later. The main risk factors associated with 9/11 were:
- Intense dust cloud exposure
- Returning to a home with a heavy layer of dust
- Witnessing horror
- Job loss
- Lack of social support
Firefighter PTSD Statistics
Studies have shown that anywhere between around 7% and 37% of firefighters meet the criteria for a current PTSD diagnosis.

World War 2 PTSD Prevalence
Among individuals who had previously sought psychiatric treatment, 37% of the World War 2 veterans and 80% of the Korean War veterans had current PTSD. It was found that 54% of a group of psychiatric patients who had been in combat during World War 2 met criteria for PTSD. At the time, the prevalence for PTSD was 27%.

Frequently Asked Questions
What is PTSD?
PTSD stands for post-traumatic stress disorder, and the disorder develops in some who have experienced a dangerous or shocking event and have a challenging time recovering from the trauma the incident caused.
Life-threatening events are common risk factors for PTSD. For example, military personnel who have experienced violence, people who have lived through natural disasters, victims of sexual abuse, and those who were involved in a car accident have an unfortunate high chance for developing the disorder.
What does PTSD do to a person?
People diagnosed with PTSD have disturbing, intense thoughts and feelings related to their experience that can last long after the traumatic event occurred. They may even relive the event through nightmares or flashbacks, they may feel sadness or even depression, anger, fear, and they may feel detached from others.
What are 3 things that can lead to PTSD?
Here are the most common events that can lead to PTSD:
- Physical or sexual assault
- Serious accidents
- Abuse, including childhood or domestic abuse
How long does PTSD last for?
Some people with PTSD recover within just 6 months, while others have symptoms that can last much longer. In some people, the condition becomes chronic and can result in depression and anxiety. A doctor, such as a psychologist or psychiatrist, who has experience helping people with mental illnesses can diagnose PTSD.
Is PTSD a cause of death?
Post-traumatic stress disorder more than doubles a veteran’s risk of death from any cause. It’s also an independent risk factor for cardiovascular disease, according to research presented in 2010 at the American Heart Association’s Scientific Sessions.
Can PTSD change your personality?
Yes, a study published by the National Library of Medicine concluded that PTSD is a risk of development enduring personality changes with serious individual and social consequences.
Can PTSD be cured?
As with the majority of mental illnesses, no cure exists for PTSD. However, it’s possible to effectively manage the symptoms to help the affected individual restore themself to normal functioning. A combination of therapy and medication is the best hope for treating the disorder.
Does PTSD affect memory?
If you have PTSD, you might notice that it’s challenging for you to concentrate or that you have memory issues such as memory loss. In fact, memory and concentration problems are common symptoms of PTSD.
Can PTSD last a lifetime?
As with the majority of mental illnesses, PTSD is very personal and no two cases are the same. In fact, according to Dr. Kriegeskotten, “When PTSD is not treated, it can last a very long time, perhaps a lifetime.”
PTSD Research & Sources
- Post-traumatic stress disorder
- National Center for PTSD
- Post-traumatic stress disorder
- Diagnosis and management of post-traumatic stress disorder
- Epidemiology of PTSD
- PTSD and Veterans: Exploring The Statistics
- Post Traumatic Stress

Have Any Questions?
Whether you're curious about our services or need support, we're just a click away. Reach out or check our FAQs for quick answers.

